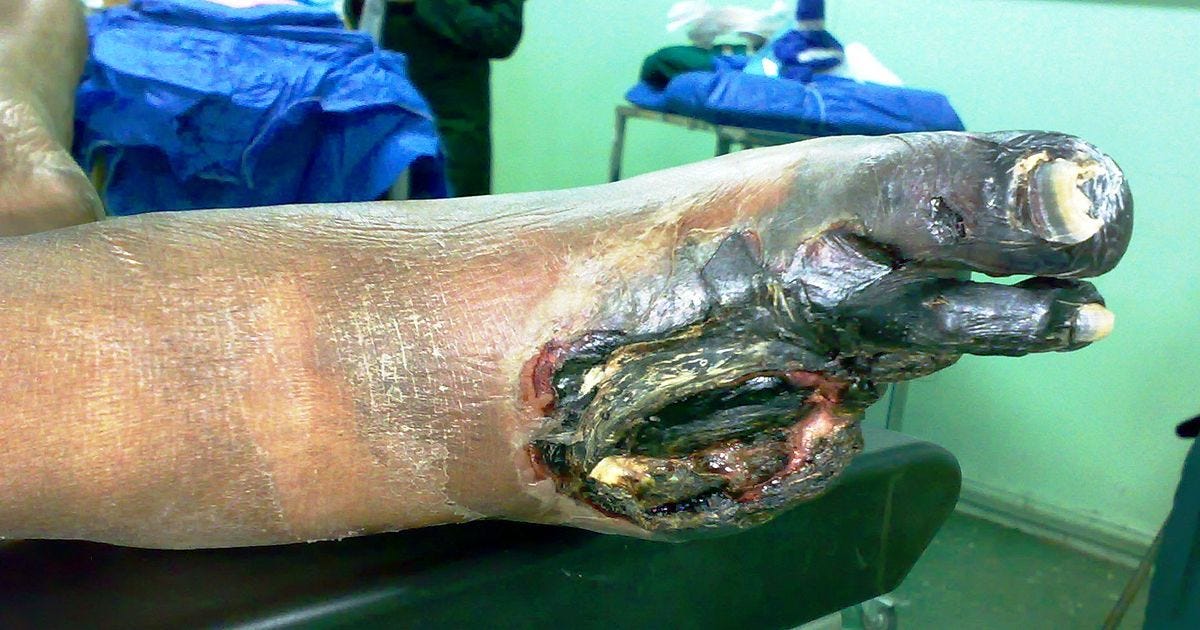
This image is horrific and I thought more than twice about using it, but I think it is critical for everyone to understand the stakes in this discussion. Every case of gangrene, every amputation is a failure. It may be a patient failure to find a primary care doctor and have their sugar and blood pressure measured. They may not know they are at risk. If the health system did the right thing and helped the patient understand her disease, developed a long-term supportive relationship, and provided optimal medical therapy and support for the patient at risk, failure is on the patient. More frequently, the patient does not get that level of care and it is on the provider system.
Payment priorities drive provider system performance and now the Medicare system is changing the codes for peripheral arterial disease so that the payer only gets a higher risk adjustment if rest pain exists with PAD patients. Rest pain is extremely late disease--just before gangrene. The vascular disease is so bad the poor patient has pain when she is totally inactive—doing nothing. She can’t do anything. If she tries to walk, the pain is quickly worse. By this time both macrovascular and microvascular disease exists, the cat is out of the barn, and our ability to modify the course is much reduced. Usually reaching this point reflects medical system failure, and they certainly should not be paid more for a failure. The legal term is “knew or should have known.” We are in an open comment period for this legislation, and if you could take the time to make a comment that could really help.
This policy statement from the American Heart Association is less than a year old.
"Among patients with diagnosed PAD (leg artery disease that causes amputation), ≈11% are likely to develop critical limb ischemia (lack of blood flow) (CLI; also known as chronic limb-threatening ischemia), a clinical condition in which the blood supply to the limb does not accommodate the resting metabolic needs of the tissue, resulting in persistent foot pain, skin ulceration, and gangrene"
This is an increasing problem. From 2009 to 2015 the amputation rate in Americans with diabetes increased by fifty percent after falling for years. Yes, you read it right. Fifty percent more people are having amputations because our system is not providing the optimal medical therapy that they need.
Patients with rest pain and critical limb ischemia are extremely high risk " Critical limb ischemia increases the risks of limb loss and mortality. Patients with CLI have a major amputation rate as high as 40% at 6 months and a mortality rate of 20% to 25% in the first year after presentation." Once rest pain develops, nearly half lose a leg and a fourth are dead in 12 months.
The AHA policy statement listed above shoots for a 20% reduction in leg amputation over the next ten years. Proof already exists that OMT can reduce amputation three fold over thirteen years. That is not a fractional improvement. It is a multiple improvement. It is important to realize that achieving that remarkable result requires early intervention. In this important study, both the OMT group and the usual care group went on OMT after 8 years. The early OMT group continued to do much better. At 13 years, with 80 patients in each arm of the study, there were 10 amputation events in the OMT group and 33 in the usual care group.
If a patient is engaged with a health system and develops rest pain, the responsible system should be penalized, not rewarded. OMT is even better now and they failed to provide OMT, the best evidence-based care. The patient's vascular disease started decades before when they developed high blood pressure and /or diabetes and/or started smoking. Proof exists that if we address those conditions with OMT early, amputation is one third as common. That is what we should reward, not sitting on your hands for decades.
Let's help get this message in front of the Medicare people.
The communication is from CMS. Below is the link to the CMS Advance Notice:https://www.cms.gov/files/document/2024-advance-notice.pdf
To submit comments or questions electronically, go to
https://www.regulations.gov
, enter the docket number “CMS-2023-0010” in the “Search” field, and follow the instructions for “submitting a comment.”
Comments will be made public, so submitters should not include any confidential or personal information.



This comment is from Dr. Mary O'Connor previously head of Orthopedics at Yale and founder of Vori Health
Bill,
If you care to add to your excellent post:
As an orthopedic surgeon, I have performed so many amputations for this type of foot. The level of amputation is below the knee. Performing an amputation of the front part of the foot is not the standard of care because the risk of the wound not healing---due to the poor blood supply that created the ulcer in the first place—is so high. With an amputation below the knee the patient must be fit for a prosthesis in order to walk without crutches or a walker. The cost of a below the knee prosthesis ranges from $3-24K. And prostheses need maintenance and replaced after some years. And there is the cost of rehab, so that patient can learn how to put on and take off the artificial leg prosthesis and walk with it.
Prevention is so much better than this.
Thank you for this wake up call! I would like to share this in my class. We are going over the disparities that plague our communities. Thanks again for your informative post. Much gratitude, Athena T :)