We can’t really do anything about it. We can give fluid pills and make people more comfortable, but we can’t keep them out of the hospital, and we can’t prolong their lives. That is the current understanding of this type of heart failure in usual care. That is a problem because half of all CHF patients have preserved ejection fraction or pumping function. That matters because heart failure is very dangerous, it generates one third of all Medicare spending and half the Medicare readmissions to the hospital. Eleven percent of the Medicare population over 65 has been diagnosed with heart failure. Nearly 40% of Medicare patients ultimately die of CHF.
It is an important topic for every American because of the cost to Medicare, but also because this type of heart failure is part of the aging process. If you live long enough you will very likely have it, and many of us will die from it. Diabetes, high blood pressure, and heart artery disease increase the risk, but it also occurs as part of the normal aging process. As we age, even without those risk factors, the heart gets bigger and scar tissue forms. Because of the scarring, the heart cannot fill as well, and the amount of blood ejected with each stroke is reduced. Because the pumping function is reduced, people with this condition may be very limited in their ability to exercise. They are fatigued and often short of breath. They may be in the hospital frequently.
Optimal medical therapy for type 2 diabetes started at an average age of 55, reduced hospitalizations for heart failure by 70% over two decades when compared with usual care. That is an astonishing fact and I have never seen anything like it. After 8 years, the usual care patients went on optimal medical therapy, because the benefits were so dramatic, and it was considered unethical to deny them OMT. Even so, twenty years out the differences persisted for patients who received OMT early. The investigators in the study estimated normal heart blood ejection per beat of 67% (anything over 50 is normal) in both groups when the study began.
Think of the benefit of reducing heart failure hospitalizations by 70%. Think of the improvement in health and reduction in cost that fact reflects. The best news of all is this. We now understand how OMT works to reduce hospitalization rates in these patients. OMT patients in this study all received ACE inhibitors like lisinopril or ARBS like losartan for chronic kidney disease, atorvastatin for their very high risk of heart attack and stroke, metformin for their diabetes, and aspirin to prevent clot. These medications all switch on the master genetic metabolic switch mTOR and they switch off AMPK. Spironolactone and the SGLT2 inhibitors like empagliflozin (Jardiance) also have this effect and would be added to the latest OMT regimen. The type 2 diabetes medication empagliflozin alone reduced admissions for this type of heart failure by 27% regardless of whether the patients had diabetes or not. A third of these heart failure patients have resistant hypertension. That is hypertension not controlled by a combination of lisinopril or losartan, amlodipine, and a diuretic. Adding spironolactone to the regimen in these patients dramatically lowers the pressure and reduces hospitalizations by 31%. A program designed in the late 90s reduced heart failure admissions by 70%. New medications and understanding can produce even better results, but we need to get started. Please do what you can to make OMT the standard of care in your community. Join our improvement community and subscribe.

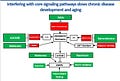


Heart failure can be eliminated if early detection of its root causes are identified, effectively treated, and monitored. Primary Lifestyle Optimization and Prevention are the keys to stop heart failure before it’s too late.