This past Friday I was on a call aimed at producing weight loss in a city. I am personally optimistic that we can accomplish that and it is very important. Excessive abdominal weight has deadly consequences. During the course of the call, I learned that the medical people involved all had some skin in the game. I weighed 303 pounds 20 years ago and I am 50 pounds lighter. Another participant weighed 330 and he is no longer too heavy. Another has a brother with weight problems who has serious related illness and he is making progress. I am an internist and I met very few patients who wanted to be fat or sick and yet successful weight loss is uncommon. The messages we all hear could not be more confusing. There are all kinds of recommendations and most of them do nothing. At a community level, we must reduce confusion and help residents understand the new science of weight loss. Sixty percent of my patients lost weight. Four lost over 100 pounds and the champ lost 150 pounds and she is still a size 8. Practical solutions exist now.
I promise you I hated being too heavy. It was a barrier to my effectiveness as a physician. I was advising people on lifestyle and my lifestyle failure could not be hidden. I would talk about weight loss and patients would just smile. It was not as if I wasn’t trying. I was doing just what the “experts” recommended. I would try to cut back on the food I was eating and I could do it for a month or six weeks, but it was like holding my head underwater. I would lose twenty pounds and when I came up for air, I would gain twenty-five. I tried a low fat diet and I replaced the fat with processed carbs. No help. I should point out here that obesity is not a sign of a deep psychological flaw, personal weakness, of lack of willpower. It is a food disease.
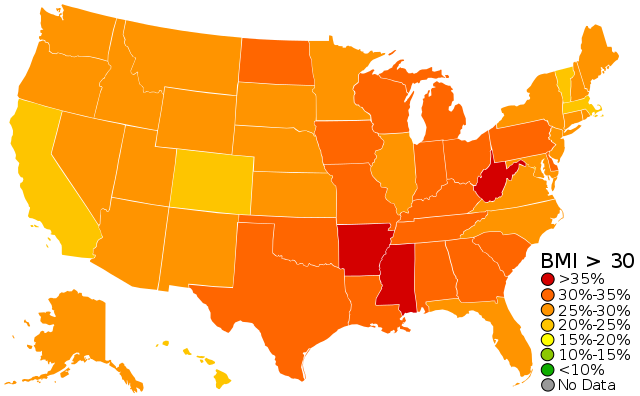
The fundamental problem was I grew up in South Carolina. Look at the map. Obesity rates are higher in the Southeast and this is a cultural issue. Long before the fast food and processed food craze hit America, sweet tea was the everyday drink in the south. This drink contains one cup of sugar for every four cups of water. There was a pitcher of sweet tea in our refrigerator at all times and I loved it. Southern cooks also knew the secret of addictive food 100 years ago. Combinations of fat, salt, sugar, and processed carbs are irresistible. Think fried chicken, mashed potatos and gravy, macacroni and cheese, biscuits, peach cobbler, and sweet tea. I have eaten many meals like that. Over the last 50 years, fast and processed food producers have learned how to do the same thing-burgers, fries, milkshakes. This food is addictive. Many of us will eat it when we are not hungry. The more we eat, the more we want. That is the root cause of obesity. Obesity is a food disease. You can’t outrun a spoon. Once I learned that, I made progress with my weight and you can too.
Obesity is a food disease. You can lose a pound or two a month by changing what you eat. It is not a diet. You can go crazy once a week at the birthday party or tailgate and be part of the fun. You can eat to live all week and live to eat one meal. You don’t have to be perfect, but most of the time, you must eat real food—lean meat, eggs, dairy products, fruits, vegetables, beans, peas, and nuts. Avoid sugar except at that one meal like it is poison (it is), and watch your health slowly improve.
Honestly, medicine has been part of the problems. Doctors prescribe medications that cause weight gain and then blame patients because they don’t lose weight. Anything that raises the insulin level causes weight gain. That includes medications like glyburide and glipizide. Type 2 diabetes is a weight disease. Using medications that cause weight gain is irrational unless there is no alternative. We have medications that favor weight loss. Use them. Beta blockers for hypertension cause weight gain. Avoid them unless there is some compelling reason to use them. Some antidepressants and antipsychotics cause weight gain. Use alternatives if you can. On the other hand, medications like empagliflozin (Jardiance) and liraglutide (Saxenda) favor weight loss and Saxenda is approved for that indication. Our approach to cardiometabolic conditions should be weight-centric.
These measures will turn the tide in most people. I told you 60 percent of my patients lost weight. There was a clue in the other 40%. I treated many couples. If the spouse lost weight, the other spouse almost always lost weight and vise versa. If the food culture in the home did not change, the weight just continued to increase. Changing the food culture works consistently.
If these measures fail, then and only then should we consider a surgical approach with a gastric sleeve or bypass. If patients don’t change what they eat, they can still relapse and complications with surgery are common. I needed extensive abdominal surgery for cancer 30 years ago. As part of the healing process, scar always forms and that can lead to bowel obstruction which is very painful and can lead to hospitalizations, repeat surgery—and more scar formation. I have had a partial bowel obstruction twice a year for thirty years and they were all miserable. Give yourself a chance to avoid surgery if you can. I know you can do it! Give it a try and let me know if you make progress. I would love to share your important story. 423-782-0372 wbestermann@congruityhealth.org



I lost the weight 2 years ago and kept it off until recently. I’ve added Kind bars to my food repertoire, and I’ve also added Crestor after my stroke. I’m unusually tired and fatigued, too. Thank you for your interest.
This is very instructive and encouraging, Bill. After losing 50 pounds, I’m seeing the scale climb again and need to intervene before I gain it back.