Most patients and healthcare professionals think of Type 2 diabetes as a sugar problem. And indeed, that is the way it is defined by the current medical model. If your fasting sugar is 126 or higher, you have diabetes. If it is under 126 you don’t. If you have diagnosis of diabetes and your fasting sugar falls below 126 consistently off medication for diabetes, you diabetes has been “reversed”. The selection of 126 as the cutoff is based on old data about diabetes complications.
That way of thinking about diabetes is not consistent with the latest scientific knowledge. Patients with abnormally high sugar don’t die of glucose elevation. They die of heart attack, stroke, chronic kidney disease, and heart failure. They die of cardiovascular disease. Patients with prediabetes (fasting sugar of 100-125) have an increased risk of these cardiovascular complications. That increased risk extends even down into the normal sugar range.
The other deviation from the latest scientific knowledge comes from thinking of diabetes as an isolated risk factor. In 1988, at about the same time that scientists were beginning to understand that chronic heart artery blockages don’t cause heart attacks, Dr. Gerald Reaven understood that obesity, insulin resistance, high blood pressure, high LDL-cholesterol, low HDL cholesterol, high triglycerides, diabetes and cardiovascular complications are all related. But old scientific dogma is difficult to overcome, and nearly twenty years later the American Diabetes Association and The European Association for the Study of Diabetes issued a joint statement:
“While there is no question that certain CVD risk factors are prone to cluster, we found that the metabolic syndrome has been imprecisely defined, there is a lack of certainty regarding its pathogenesis, and there is considerable doubt regarding its value as a CVD risk marker. Our analysis indicates that too much critically important information is missing to warrant its designation as a “syndrome.” Until much needed research is completed, clinicians should evaluate and treat all CVD risk factors without regard to whether a patient meets the criteria for diagnosis of the “metabolic syndrome.”
So, as recently as 2005, the most prestigious diabetologists and advocacy organizations for diabetes drew a line in the sand. Stick to the old risk factor model. That is a real problem because even the idea of the metabolic syndrome falls far short of the new scientific reality. It is not just the cardiovascular risk factors that are related. The same epigenetics, excess oxidants, and signaling drive the speed of chronic disease development and the rate of aging.
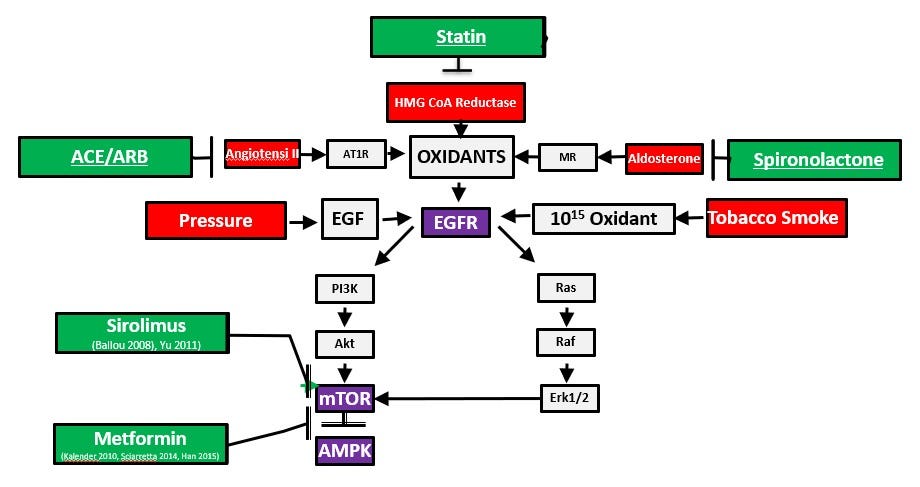
As you can easily see from this diagram, the idea of the metabolic syndrome does not go far enough. The genetic signature of cardiovascular disease and cancer are powerfully related. Both diseases are due to inappropriate activation of the same gene networks. This is a signaling diagram that works like dominoes. The arrows indicate activation or switching a gene on.
Let’s just look at one example of the power of this diagram. Abdominal fat causes excessive aldosterone production (upper right corner). The old science understands that aldosterone is a hormone that retains fluid and salt when an individual is dehydrate to maintain the blood pressure. That is like saying Tom Brady plays football or Pavoratti sings. It is true, but there is so much more to the story. Aldosterone (and cortisol) engage the MR (mineralocorticoid receptor) on the cell surface to dramatically increase oxidant production. Excess oxidant production is a critical biochemical cause of aging, cardiovascular disease, diabetes, and cancer.
The excess oxidants activate (transactivate) the epidermal growth factor receptor (EGFR) in the purple box. The EGFR is a master metabolic switch activated by oxidants, tobacco smoke and several growth factors. The receptors for many other growth factors, including insulin, can be substituted in that purple box. In insulin resistance, insulin signaling through the PI3K and AKT boxes is impaired, and insulin levels increase to overcome that impairment. Ras and Raf signaling are not impaired so growth factors more powerfully activate the master metabolic switch mTOR (mechanistic target of rapamycin) and deactivate AMPK (AMP-kinase).
The end result of increased aldosterone release related to abdominal fat is switched on mTOR and switched off AMPK. That increases insulin resistance, inflammation, cell growth as scar and cancer, and cell death that causes insulin deficiency and emphysema. These are the central signaling pathways not only for diabetes but also for cancer and cardiovascular disease. Aging and all chronic diseases involve these pathways.
mTOR and AMPK coordinate food supply with normal growth in the fetus and child. When food is plentiful, mTOR is maximally activated and AMPK is switched off to support growth. When there is no food, AMPK is switched on to promote breakdown of fat and muscle to provide energy to support fetal and organ survival. The medications in the green boxes protect cells and organs by inducing a state of fasting mimicry. The effect of switching on AMPK and switching off mTOR is similar to fasting or restricting calories which are well known to prolong life and delay chronic illness.
The green box medications that mimic caloric restriction switch off mTOR and switch on AMPK. Insulin is a powerful growth factor. Insulin, and medications like glyburide that increase insulin levels, switch on mTOR and switch off AMPK to increase insulin resistance and then insulin levels in a vicious cycle. That may be why the clinical trials under the old model never lowered the risk of heart attack, stroke, and death. On the other hand, when the green box medications are included in a protocol for high risk diabetes, the risk of heart attack, stroke, and death are dramatically reduced.
Type 2 diabetes is a sugar problem, but it is so much more. It is just one piece of the abnormal metabolism that causes faster aging, cardiovascular disease, and cancer. Human beings are whole bodies of cells and organs. When we finally begin to treat the whole patient in advanced primary care teams focused on the molecular biology of chronic disease and aging, we will prolong healthy lives and reduce healthcare costs. It’s time!




Doctor, what is your opinion of that drug being given for insulin resistance. I have a friend who has a rather large abdomen and trunk area as she’s gotten older. (81). Her doc gave her this “new” med for “insulin resistance “ so she can lose weight. As far as I know there was no dietary information or lifestyle recommendations given to her. Side effects? No testing. Is this just the new weight loss thing now? Diabetes meds? Yet I couldn’t get an Rx for ivermectin. This med might be good use for this but I’m so suspicious of medicine now ....... I want to be prepared. I never express my opinions to her however.